- Visibility 180 Views
- Downloads 29 Downloads
- DOI 10.18231/j.ijooo.2024.037
-
CrossMark
- Citation
A clinicopathological study of eyelid tumors at a tertiary care hospital in South India
Introduction
An eyelid tumor leads to functional problems and cosmetic problems of the eyelid. The prevalence and distribution of eyelid tumors have considerable variation. Eyelid tumors are common in people of both sexes and all age groups representing more than 90% of ophthalmic tumors.[1] Most of the tumors are diagnosed clinically and treatment depends on the site, extent of spread and invasiveness of the tumor.
Usually majority of these cases are either inflammatory or non-malignant tumors, however many malignancies can mimic benign neoplasms and need differentiation before definitive therapy is started.[2] We should have a high suspicion when the lid tumor is slowly enlarging, associated with loss of eyelashes, prominent blood vessels, pigmentation and ulceration.[3] Histopathology remains the confirmatory and mainstay of diagnosis in cases of eyelid tumors. [4], [5]
Materials and Methods
The present study was a prospective study conducted on patients who presented with eyelid tumors to the Department of Ophthalmology, McGann District Teaching hospital, Shimoga from November 2022 to October 2024. 50 cases were included in the study, including both benign and malignant eyelid tumors.
Inclusion criteria
Patients who presented with primary tumors of eyelid.
Patients who were willing to undergo surgery.
Patients who were willing to come for follow up.
Exclusion criteria
Patients having lid swelling secondary to infectious lesion like stye, molluscum contagiosum, chalazion and pyogenic granuloma were excluded.
Patients with previously resected eyelid tumors.
After taking Informed consent from the patients, all the patients were subjected to detailed general and ocular history taking and examination. Tumours were diagnosed clinically and treatment was planned according to the nature of the lesion. Benign lid tumours were treated by surgical excision of the tumour. Eyelid tumors in lid margins were excised by shave excision and cystic eyelid lesions were excised in toto and sent for histopathological examination. Clinically suspected malignant lid tumours were treated with wide local excision and lid reconstruction after histopathological examination for margin clearance. Wide local excision of 4 mm clear margin from the clinically palpable extent of lid tumour was done in pentagonal shape. In cases with defects less than 30%, direct suturing of the lid with or without canthotomy/ cantholysis was done. In cases with defects 30-60%, lid was reconstructed by Tenzels semicircular flap technique. In cases with defects more than 60% lid reconstruction was done with mucous membrane graft from nasal septum/ periosteal reflected flap for posterior lamellae and sliding skin flap for anterior lamellar reconstruction ([Figure 1]). For confirmation of diagnosis, all excised specimens were sent for histopathological examination. Patients were on regular follow up to look for any recurrences.
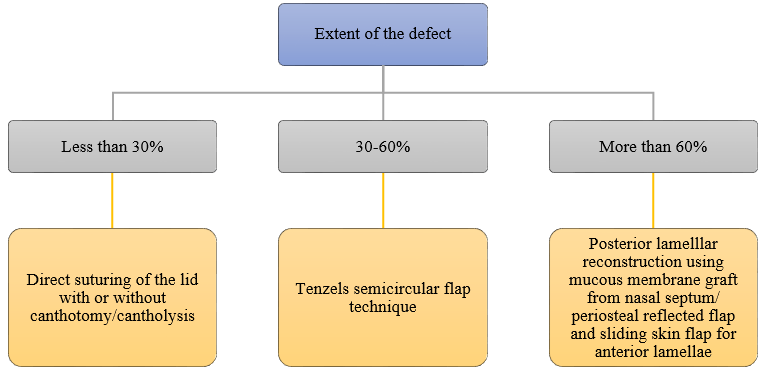
The cases were analyzed for their age group distribution, sex distribution, incidence of malignant and benign tumors, tumor location, tumor type distribution and complications at the time of presentation.
Results
In our study involving 50 patients with eyelid tumors, mean age of presentation of benign eyelid tumors was 44.81 years and mean age of presentation of malignant eyelid tumors was 67.25 years. ([Table 1]) shows age distribution of patients.
|
Age group |
Type of tumor |
Total No. of cases |
|
|
Benign |
Malignant |
||
|
11-20 |
1 |
- |
1 |
|
21-30 |
7 |
- |
7 |
|
31-40 |
12 |
- |
12 |
|
41-50 |
9 |
- |
9 |
|
51-60 |
9 |
1 |
10 |
|
61-70 |
7 |
1 |
8 |
|
71-80 |
2 |
1 |
3 |
|
Total |
47 |
3 |
50 |
Among all cases 29 were females and 21 were males. Both benign and malignant lid tumors were more commonly seen in females. ([Table 2]) shows sex distribution of patients.
|
Sex |
No. of patients |
Percentage |
|
Male |
21 |
42% |
|
Female |
29 |
58% |
|
Total |
50 |
100% |
Among 50 cases of eyelid tumors 47 cases were benign and 3 cases were malignant. ([Table 3]) shows distribution of cases according to type of lesion.
|
Type of lesion |
No. of cases |
Percentage |
|
Benign |
47 |
94% |
|
Malignant |
3 |
6% |
|
Total |
50 |
100% |
Among all cases of eyelid tumors, upper lid involvement was seen in 38 cases and lower lid involvement was seen in 12 cases. Benign tumors were more commonly seen involving upper eyelid. ([Table 4]) shows distribution of eyelid tumors based on their location.
|
Tumor location |
Benign |
Malignant |
Total cases |
Percentage |
|
Upper lid |
37 |
1 |
38 |
76% |
|
Lower lid |
10 |
2 |
12 |
24% |
Intradermal nevus ([Figure 2]) was the most common benign tumor seen with 15 cases followed by epidermal cyst ([Figure 3]) seen in 13 cases. Eccrine hidrocystoma, seborrheic keratosis ([Figure 4]), papilloma, cyst of moll, fibroepithelial polyp, keratinous cyst, eccrine spiradenoma ([Figure 5]), hemangioma, pilomatricoma and schwannoma were the other benign eyelid tumors seen. ([Table 5]) shows incidence of benign tumors.




|
Type |
Number |
% |
|
Cyst of moll |
2 |
4.25 |
|
Eccrine hidrocystoma |
3 |
6.38 |
|
Eccrine spiradenoma |
1 |
2.12 |
|
Epidermal cyst |
13 |
27.65 |
|
Fibroepithelial polyp |
2 |
4.25 |
|
Hemangioma |
1 |
2.12 |
|
Intradermal nevus |
15 |
31.92 |
|
Keratinous cyst |
2 |
4.25 |
|
Papilloma |
3 |
6.38 |
|
Pilomatricoma |
1 |
2.12 |
|
Schwannoma |
1 |
2.12 |
|
Seborrheic keratosis |
3 |
6.38 |
|
Total |
47 |
100 |
All the 3 malignant tumors seen were sebaceous gland carcinoma. Among the three sebaceous gland carcinoma two were females involving lower eyelid and one was male involving the upper eyelid ([Figure 6], [Figure 7], [Figure 8]).
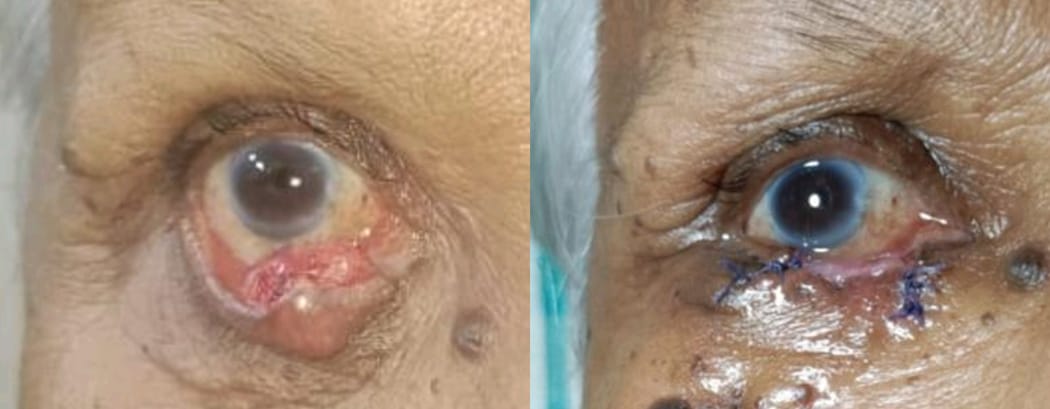
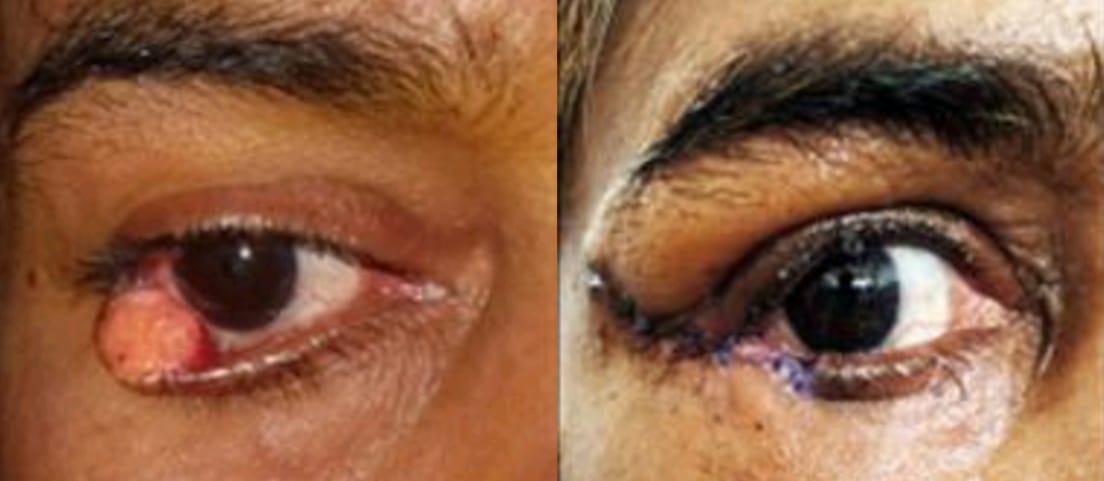
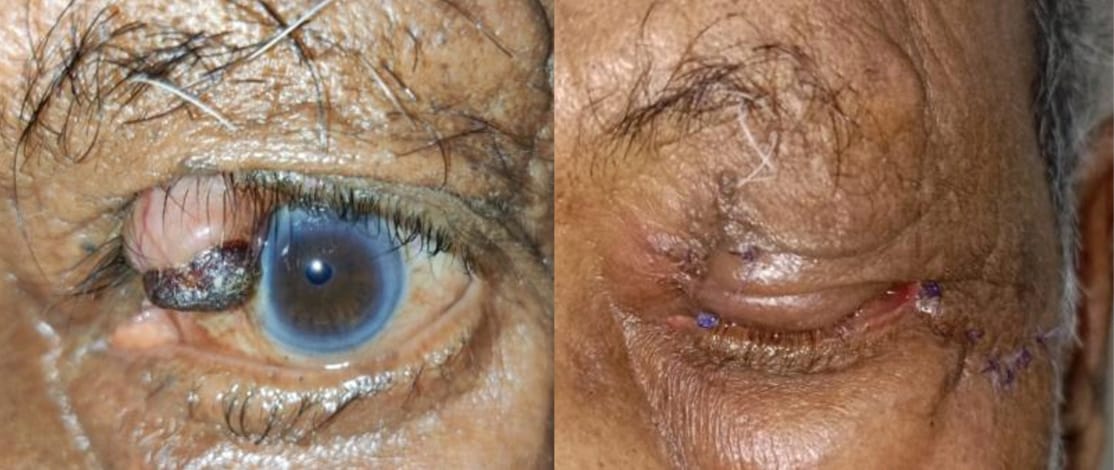
Discussion
Eyelid tumors, in addition to impacting the cosmetic appearance of the face and disturbing the normal structure and function of the eyelid, are significant contributors to both morbidity and mortality. Based on literature review, it is conclusive that malignant tumors are less common than benign lesions. In our study, 94% lesions were benign growths and 6% were malignant tumors, consistent with studies by Deswal et al.[6] and Karan S et al.[2] In another study conducted by Krishnamurthy et al. in Karnataka 91.9% of cases were benign and 8.1% cases were malignant eyelid tumors. [7]
The mean age of presentation of benign tumors was 44.81 years and malignant tumor was 67.25 years, similar to Mary Ho et al. [8] Rathod et al. reported 100 cases of eyelid tumors where mean age of presentation of benign tumors was 37.02±16.84years and malignant eyelid tumors was 58.59±11.27 years. [1] Hence, this supports the fact that with increasing age, the risk of malignant tumor of eyelids increases.
In our study, both benign and malignant lesions were more common in females, with male to female ratio of 1:1.3 as same as study by Bhavya P Mohan and Letha V.[9] In present study the benign lesions were more commonly seen in upper eyelid and on the other hand, malignant tumors were seen more commonly on lower eyelid consistent with Deswal et al. study. [6]
Most common benign eyelid tumors seen in our study was intradermal nevus with 15 cases (31.9%) followed by epidermal cyst with 13 cases (27.6%). In a study by Rathod et al. intradermal nevus was the most common benign lesion with 27.8%.(1) In Nithithanaphat C et al. study intradermal nevus was the most common benign lid tumor.[10] In Krishnamurthy et al. study done in Karnataka epidermal cyst was the most common eyelid tumor followed by nevi.[7] Rare benign eyelid tumors seen in our study were eccrine spiradenoma and schwannoma.
Eccrine spiradenoma is a rare benign sweat gland tumor, usually presents as solitary, intradermal and painful nodule, occasionaly it presents with lobulated appearance. Histologically tumor comprising lobules of various sizes in the corium with basophilia confined to dermis is seen. [11], [12] Schwannoma is a rare benign tumor of peripheral nerve origin. It usually presents as slowly enlarging, solitary, painless mass. Histologically tumor comprising fusiform cells arranged in interwined bundles where the nuclei is fusiform and form palisades is seen.[13] In both eccrine spiradenoma and schwannoma, incomplete removal is associated with eventual recurrence and aggressive behaviour.
Among malignant eyelid tumors in our study, all three of them were sebaceous gland carcinoma. Karan et al. Mohan BP et al. and Krishnamurthy H et al. studies also show sebaceous gland carcinoma as the most common malignant eyelid lesion similar to our study.[2], [7], [9] Though the most common malignant tumor of the eyelid worldwide is basal cell carcinoma, sebaceous gland carcinoma is more common in Asian countries with an increasing trend. [14], [15], [16]
Among all the cases, one case of benign eyelid tumor presented with complications like pigmentation, ulceration over the swelling with loss of eyelashes at time of presentation, hence it was clinically diagnosed and treated as malignant lid tumor but histopathology of excised specimen revealed it to be eccrine spiradenoma (Figure 4). Among all three malignant lid tumors, two of them presented with ulceration and loss of eyelashes at the time of presentation and the third case presented with loss of eyelashes and hemorrhage from the lid tumor at the time of presentation, hence all of them were diagnosed as malignant lid tumor clinically.
During follow-up period, a case of sebaceous gland carcinoma (case 2) developed pyogenic granuloma at the site of excision, after duration of around 5 weeks, which subsided after treatment with topical medication. Rest of the cases of eyelid tumors did not have any postoperative complictaions. One case of epidermal cyst presented with recurrence of swelling at the same site after a duration of around one year.
Conclusion
Intradermal nevus and epidermal cyst are the most common benign eyelid tumors and Sebaceous gland carcinoma is the most common malignant eyelid tumor. Histopathological examination of all excised eyelid tumors is essential, as they may be malignant and require definitive treatment for better long-term management of the patient. Eyelid tumor that show secondary changes such as pigmentation, ulceration, loss of eyelashes, or bleeding should be treated as early as possible with wide local excision, as the likelihood of malignancy is significantly high in such cases. Having knowledge and insight of various eyelid lesions, particularly rare ones, enhances the ability to provide better patient care.
Limitations
Limitations of this study were small sample size and difficulty in follow up.
Ethical Committee Approval
Taken. SIMS/IEC/883.
Consent
Prior to the study, informed consent was obtained from all participants. They were fully briefed on the study details, with a clear assurance that their personal information would remain confidential and that any photos taken during the study would be used in a way that will not reveal their identity. Participants who voluntarily agreed to participate, understanding these terms were included in the study.
Conflict of interest
None.
Source of funding
None.
References
- A Rathod, M Pandharpukar, K Toopalli, S Bele. A clinicopathological study of eyelid tumors and its management at a tertiary eye care centre of Southern India. MRIMS J Health Sci 2015. [Google Scholar] [Crossref]
- S Karan, M Nathani, T Khan, S Ireni, A Khader. Clinicopathological study of eyelid tumors in Hyderabad - A review of 57 cases. J Med Allied Sci 2016. [Google Scholar]
- S Paul, D T Vo, R Silkiss. Malignant and benign eyelid lesions in San Francisco: study of a diverse urban population. American J Clin Med 2011. [Google Scholar]
- BE Cook-Jr, GB Bartley. Treatment options and future prospects for the management of eyelid malignancies: an evidence-based update. Ophthalmology 2001. [Google Scholar]
- J P Hilovsky. Lid lesions suspected of malignancy. J Am Optom Assoc 1995. [Google Scholar]
- J Deswal, N Anand, A K Khurana. Profile of eyelid tumors at a tertiary eye care hospital in North India- a 3-year retrospective study. J Evid Based Med Healthc 2020. [Google Scholar]
- H Krishnamurthy, V Tanushree, H T Venkategowda, S Archana, G Mobin. Profile of eyelid tumors at a tertiary care institute in Karnataka: a 5-year survey. J Evol Med Dent Sci 2014. [Google Scholar]
- M Ho, DTI Liu, KKL Chong, HK Ng, DSC Lam. Eyelid tumours and pseudotumours in Hong Kong: a ten-year experience. Hong Kong Med J 2013. [Google Scholar]
- BP Mohan, V Letha. Profile of eye lid lesions over a decade: a histopathological study from a tertiary care center in South India. Int J Adv Med 2017. [Google Scholar]
- C Nithithanaphat, S Ausayakhun, D Wiwatwongwana, P Mahanupab. Histopathological diagnosis of eyelid tumors in Chiang Mai University Hospital. J Med Assoc Thai 2014. [Google Scholar]
- BK Ahluwalia, AK Khurana, AD Chugh, VG Mehtani. Eccrine spiradenoma of eyelid: case report. Br J Ophthalmol 1986. [Google Scholar]
- SS Pal, MS Alam. Eccrine spiradenoma of eyelid - A rare tumor at an unusual location with literature review. Orbit 2024. [Google Scholar] [Crossref]
- SB Patil, SM Kale, S Jaiswal, N Khare. Schwannoma of upper eyelid: A rare differential diagnosis of eyelid swellings. Indian J Plast Surg 2010. [Google Scholar]
- M Deprez, S Uffer. Clinicopathological features of eyelid skin tumors: a retrospective study of 5504 cases and review of literature. Am J Dermatopathol 2009. [Google Scholar]
- R Paul, MN Islam, E Kabir, HR Khan, UK Kundu. Tumors of the eyelid: a histopathological study at tertiary care hospitals in Dhaka, Bangladesh. IMC J Med Sci 2017. [Google Scholar]
- MC Coroi, E Rosca, G Mutiu, T Coroi, M Bonta. Eyelid tumors: histopathological and clinical study performed in County Hospital of Oradea between 2000-2007. Rom J Morphol Embryol 2010. [Google Scholar]
